National framework for the delivery of bereavement care
This framework supports those commissioning or providing bereavement services. This is to ensure that good quality services are available for those who need them.
In this page
1. Ministerial foreword
Bereavement is something that we all have to face during our lives. Some of us may have support around us to help us cope with the grief that we feel when we lose a loved one; some may not have support; and for some additional help may be necessary.
Our vision is for a compassionate Wales where everyone has equitable access to high quality bereavement care and support to meet their needs effectively when they need it. To achieve this we must build on the excellent examples of bereavement care across Wales and address the gaps and challenges in delivering service provision that we know exist.
This bereavement framework describes how in Wales we can respond to those challenges and seeks to guide our commissioners and providers of bereavement services to ensure that there is clarity on the type and standard of support that we would like to see for bereaved people in Wales.
The framework has been developed in line with the five ways of working, in the Wellbeing of Future Generations Act and the priorities set out in the Programme for Government to provide effective, high quality and sustainable healthcare and in particular to improve service access and integration. It describes a longer-term vision along with short to medium term actions that require a collaborative approach across health, social care and the third sector. Public involvement has been key to shaping the framework, and is fundamental to the delivery of bereavement care. The framework also has a strong focus on preventive activity through the recognition of anticipatory grief and support for families, friends and carers.
To deliver on this commitment, £1.4m of additional funding is being made available to health boards and our third sector partners to support the implementation of the framework and the bereavement standards. The National Bereavement Steering Group will work with health boards, local authorities, regional partnership boards and the third sector to ensure that the framework is implemented at pace, supported by key enablers such as digital infrastructure and a skilled workforce. A robust system of monitoring and evaluation will ensure that the framework will deliver the expected benefits for the people of Wales.
Finally, I would like to thank all the individuals (many of them volunteers) and organisations who do so much to provide bereavement care and support across Wales. Their dedication and commitment to supporting people in their hour of need, is exceptional and a reminder of the compassion and kindness that we want to be available to all bereaved people in Wales.
Eluned Morgan MS
Minister for Health and Social Services
Lynne Neagle MS
Deputy Minister for Mental Health and Wellbeing
2. Policy aims andcontext
Aim of the document
This framework seeks to set out how in Wales we can respond to those who are facing, or have experienced, a bereavement. Good bereavement support should be something available to everyone who needs it. It is to some extent the responsibility of all of us, whether it is provided by our friends, families, within our communities, our health and social care systems, the voluntary sector, our work or elsewhere.
It is underpinned by a desire to make sure that we do all we can to support people affected by bereavement. This might be during the period leading up to, or following, the death of someone significant in their lives. It is intended that this framework will set the standard and be a catalyst to drive improvements in the quality, provision and availability of bereavement support across Wales.
Vision statement
Our vision is for a Compassionate Wales where everyone has equitable access to high quality bereavement care and support when they need it.
Who can use this framework?
The framework is primarily addressed to commissioners (health boards and local authorities where applicable) and providers of bereavement services, but will also be of interest to Registrars, Funeral Directors, Medical Examiners and anyone who is supporting someone who is bereaved, or who is bereaved themselves. We know that almost all bereaved people will rely on contact with people in their own communities in the first instance for the kind of compassionate support everyone can provide. We believe that recognising this, and appropriately encouraging and helping people to offer this support is an important priority for all communities and we want the framework to be part of the effort to ensure this baseline of information and kind help is valued and resourced.
Why has this guidance been developed?
This framework seeks to support commissioners and providers to understand their responsibilities to ensure the provision of equitable and timely access to high quality bereavement care and support to the local population. Bereavement provision needs to meet the differing needs of differing communities and people of all ages. This framework includes a set of bereavement standards (Annex 1) and offers a general person centred aid to planning, commissioning and delivering bereavement services.
The document has been prepared by the National Bereavement Steering Group, made up of statutory and voluntary agencies who work with people who are dying, and those who are bereaved in Wales. These agencies have taken steps to involve those with lived experience to express their particular needs and to help design services. Membership of the National Bereavement Steering Group is attached at Annex 2.
Bereavement consultation
A consultation on the draft framework ran from 22 March – 17 May 2021. 65 responses were received from private individuals and a variety of organisations, including Health Boards and Trusts, the Royal Colleges, the Children’s Commissioner for Wales, the Welsh Language Commissioner, and a variety of third sector organisations.
3. Introduction
Bereavement is something that touches all of our lives, sometimes many times over. Grief, our response when someone dies, is a natural and individual process and not an illness but its effects can sometimes be devastating.
It can happen at any age, by the death of a person at any age, and in any place. It can follow a death that is sudden for any reason, or can happen in the context of progressive illness. It can be experienced before the death and during the illness itself, or immediately after a death, or at any stage in the life of the bereaved person, whatever that person’s relationship to the person who died. Some providers of bereavement support will encounter people in particular forms of bereavement, but other providers and in particular commissioners of bereavement care will need to be mindful of all people experiencing bereavement to make sure that none is left out. In that sense, while it is addressed to commissioners and providers of bereavement care, this framework is for the people it is designed to help: people experiencing bereavement.
How we experience grief may be influenced by a number of factors including age, cultural and religious/spiritual beliefs, and our relationship with the deceased. Every bereavement experience is included in the remit of this framework. Whether we have a support network of family and friends, or feel isolated and are having to deal with family tensions, we recognise that all can have a major impact on our wellbeing in the medium to long term. Some people may derive comfort from their spiritual or religious beliefs, especially prior to and following a funeral. This support may be invaluable to them at this very difficult time and afterwards.
Bereavement can severely affect a person’s overall health and behaviour. It can trigger a range of emotions and physical symptoms which we may never have experienced before which leave us feeling lost and unable to function. It is known there are costs, often long term, associated with allowing grief to remain hidden and unsupported. Everyone at any age can suffer from these negative impacts from very young children to the oldest members of our society. Bereavement care is part of health and social care’s core work.
There are examples of good bereavement care in parts of Wales. However, there are gaps and limitations in its provision. More is provided in some parts of Wales than in others, and some groups of people experiencing bereavement in particular contexts or at particular stages of life have not been able to get the right support at the right time.
We are aware that some groups of people and communities may find accessing support difficult. It is important that commissioners and providers of bereavement services understand how the provision of, and access to, bereavement support services for Black, Asian and Minority Ethnic Communities, and people with protected characteristics could be improved. The requirement for this to take place has been included as a standard for commissioners of bereavement services.
This framework seeks to address the inequity of the response to bereavement in Wales and will support the development of networks of services and other responses, to help people regardless of where they are in Wales and across the whole range of bereavement experiences.
People in Wales have always sought to care for those who are facing the death of someone close to them. The urgent goal is to do this better and more fairly across Wales, so more people get what they need.
4. Strategic context
A Healthier Wales (2018) sets out the long-term future vision of a ‘whole system approach to Health and Social Care’ and called for bold new models of seamless local health and social care at the local and regional level. It challenged us to work differently, not just across portfolios within Government, but also with our partners and stakeholders.
The recently published National Clinical Framework provides a clinical interpretation of 'A Healthier Wales' and describes a learning health and care system, centred on clinical pathways that focus on the patient, grounded in a life-course approach.
Our third and independent sector stakeholders make an important contribution and the Welsh Government values the contribution that these sectors make to the long-term economic, social, environmental and cultural well-being of Wales, its people and its communities. In line with the principles of the Well-being of Future Generations Act this framework requires the Welsh Government and other public bodies to think about the long-term impacts of the decisions we make today for a better tomorrow. This legislation is fundamental to developing a coherent, holistic and long-term response to bereavement care in Wales.
The Social Services and Well-being (Wales) Act 2014 established the Regional Partnership Boards (RPBs), to improve the well-being of the population and to improve how health and care services are delivered. The RPBs are key to ensuring that proposals are co-produced with third and independent sector organisations, local authorities and the NHS to best meet the needs of the local population. A new Bereavement Support Grant is being established to support the implementation of the framework and RPBs will be invited to comment upon applications received for their respective areas.
The NHS Planning Framework, which is also the Minister’s direction to the NHS, always seeks to align with the Wellbeing of Future Generations Act and to continue to strengthen how organisations work to deliver their plans using the five ways of working (long term, prevention, integration, collaboration, involvement).
COVID-19 has had a profound effect upon the delivery of NHS and social care services, as well as changing the behaviour of the general public in the way they access healthcare. However, the vision we set out in 'A Healthier Wales' for seamless health and social care remains sound, with many of the new ways of working and innovative approaches introduced in response to the pandemic accelerating progress. Welsh Government remains committed to delivering the transformation needed.
Since the beginning of the COVID-19 pandemic, there has also been a strong focus on avoiding the harms that have been the key quality context within which services and care must be provided.
Welsh Government has published 'Looking Forward' to help health and social care emerge from the pandemic, describing the challenge as building the integrated health and social care service that we want going forward and to deal with the long-term impacts of COVID-19. The opportunity is to change for the better, recognising that COVID-19 is still with us.
A key aspect to this recovery is ensuring that care is as safe as possible, and that harm is minimised. The five harms we describe in health and care in Wales are:
- Direct harm from COVID-19 itself
- Indirect harm from COVID-19 due an overwhelmed health and social care system and reduction in healthcare activity as a result
- Harm from population based health protection measures i.e. educational harm
- Economic harm both directly and indirectly as a result of COVID-19 i.e. unemployment as a result of lockdown
- Harm as a result of exacerbation or introduction of new inequalities in society
The NHS Planning Framework sets an expectation of a broad approach to prevention to be applied in all aspects of planning. This is supported by Welsh Government policy that is set out from a perspective of prevention.
Preventative approaches to all physical and mental health challenges and support for wellbeing will ultimately avoid escalation of conditions and illness. Health and social care providers should consider opportunities that will support future generations and inform future service provision.
Our aim is to take significant steps to shift our approach from treatment to prevention. For bereavement, in addition to providing the best end of life care experience possible, this means providing people with appropriate and timely bereavement care and support, as delays can contribute to the development of more complex grief.
The priorities that will be delivered through the bereavement framework continue to support the principles of prudent and value based healthcare with its focus on integrated, co-produced, person centred care delivered in a way that has been informed by service users and carers.
5. Scope
Bereavement is experienced in relation to the death of a person wherever and whenever it happens. For the purpose of this framework, it includes pre-bereavement (a grief reaction before someone dies sometimes referred to as anticipatory grief) and includes bereavement experience of anyone, whatever his or her relationship to the person who dies. It includes bereavement due to the death of any person, including those who die before birth for any reason and at all gestation ages. Bereaved people may not always feel that their bereavement has been recognised, which may result in disenfranchised grief, where their grief may remain hidden because they feel it is not accepted or acknowledged by others.
All types of bereavement and pre-bereavement are included, wherever and whenever they occurred, and whatever the circumstances around the death.
There is a link between the care provided for people at the end of their lives, whether or not there are opportunities and a willingness by families to have conversations about a person’s wishes and “what matters most” to them. These conversations can be extremely helpful to families during the subsequent bereavement process, as well as being very reassuring for the person at end of life.
Where a death can be anticipated, services should work with families to help them make whatever preparations they consider necessary, engaging in open and honest communication about their needs and any concerns they may have for the care of the person at end of life, and for the wider family. This may include a discussion about any dependents they may have, adults or children, and if appropriate, a safe guarding referral made in a timely manner before their health deteriorates further, to ensure the safety and well-being of those dependants.
Ensuring that families are aware of the support available to them from elsewhere, including financial/benefits advice, practical support as well as emotional support is an essential part of helping families in these circumstances.
Staff dealing with families, who are bereaved suddenly, often in traumatic circumstances, need to recognise that the circumstances of the death may mean that their immediate needs for support and help may be different, to other types of bereavement. They will need to ensure that the family receive appropriate guidance on where to get any further support.
Support will be provided to children, young people, and adults of all ages without restriction, and must be accommodating of the needs of people of all communities and backgrounds. The needs of people with all disabilities, including preparing for, and following, the death of a loved one, must also be supported.
Support must always be available in Welsh and all referral information, assessments that may be carried out, leaflets, and support materials should similarly always be available in Welsh and English as part of the core offer to bereaved people in Wales.
Support in other languages should be made available, including British Sign Language (BSL). Staff have a responsibility towards patients, the general public and each other to promote equality and ensure patients receive an excellent standard of service that is fair, meets individual needs and treats everyone with dignity and respect. Effectively capturing the communication needs of patients with sensory loss is key.
Welsh Government works closely with health boards to ensure that the communication, information and health needs of people with a sight impairment and/or a hearing impairment are being met in line with the Equality Act 2010 and as set out in the All Wales Standards for Accessible Communication and Information for People with Sensory Loss.
Every effort should also be made to ensure that the support offered recognises the culture and beliefs of the bereaved person, including recognising the significance of the faith, religious or spiritual beliefs that the individual or family hold.
6. Principles
Wales should be a place where:
- People who are bereaved will be treated with compassion, empathy, and kindness, have their wishes, choices and beliefs listened to, considered and respected by all. Pre-bereavement will also be recognised, to offer support before the death wherever possible.
- People’s needs and grief reactions are recognised and acknowledged as being different at different times, (e.g. the need for practical help and/or emotional support). People may need to return several times for these different types of support following a bereavement.
- There is help to know where to turn for additional support when it is needed, this should be available for bereaved people affected by any cause of death, at a time and place when they can access it easily.
- The needs of bereaved people with protected characteristics, as outlined in the Equality Act 2010, of the Public Sector Equality Duty (age, disability, gender reassignment, marriage or civil partnership, pregnancy and maternity, race, religion or belief, sex, sexual orientation) are recognised.
7. The need for bereavement support
Every person’s bereavement experience is different but for some the extreme emotions which we can feel when grieving, including shock, anger, guilt, emptiness and lack of purpose, coupled with physical sensations including fluctuating appetite, weight loss or gain, sleep deprivation, and emotional episodes can be overwhelming. It is known that for some people, unresolved grief issues can lead to serious mental health difficulties and is a risk factor for suicide. Helping bereaved people to understand these feelings and learning how to cope with them on a day to day basis is an important part of supporting them at the most difficult time in their lives.
Many people find that the support of family and friends, school or colleagues may be sufficient to enable them to overcome, over time, the devastating sense of loss. For some, additional and/or more specialist bereavement support may be necessary. There may be identifiable reasons for this need, such as the circumstances of the bereavement, the nature of their relationship with the person who has died, or strains in their social or economic environment caused by family tensions or feelings of isolation and loneliness.
For some families, particularly those with children and young people, it may be because the family struggle to communicate about what is about to happen, where a child or other member of the family has a life limiting condition, or is at end of life, or has happened, and to understand how children cope with grief. For some, there will be no clearly identifiable reason but the need will be no less real.
Anticipatory grief, where a person can experience grief before a death, perhaps at the point of a diagnosis being received, is recognised as an area where people may need support. There may be many instances where people with a terminal illness do not receive a formal diagnosis, yet their decline causes great emotional distress to families.
Everyone should be aware of and be able to access the support they need, at a time and in a manner, which is best for them. For some, the consequences of being unable to access this support in a timely manner may include prolonged grief and other mental health disorders, including depression, anxiety, substance misuse (including alcohol), self-harm and increased risk of suicide. For children and young people it can present in risky behaviour, behaviour problems, school refusal, eating disorders and poor mental health outcomes. We must also consider how we support individuals who experience death or bereavement as part of their work such as health and social care staff, other third sector providers, “blue light” workers, prison officers and funeral staff.
The impact on a bereaved person’s family life and relationships can also be devastating, and it is recognised that the whole family, all those who are affected, including close friends or personal carers, should have access to support as and when they need it. (Carers may also experience long-term financial as well as emotional impacts after the death of the person they were caring for).
8. Models of bereavement support
There are a number of adult and children bereavement frameworks/models that set out a range of approaches to providing bereavement care and support. The Bereavement Scoping Survey undertaken by the Marie Curie Palliative Care Research Centre, Cardiff University, and the Wales Cancer Research Centre used the National Institute for Health and Clinical Excellence (NICE) three-component model.
The three-component model
NICE outlines a three-component model of bereavement support, complemented by a public health approach of universal/selective or targeted/intervention:
- Component 1 (universal): where information is offered regarding the experience of bereavement and people are sign-posted towards further support can be provided as part of a conversation, in written form (leaflets/factsheets) or via on-line resources. Intended to help bereaved people understand that, whilst everyone’s grief journey is unique, that there are certain emotions and physical characteristics which are an entirely normal reaction to the loss which they have experienced. These resources should help awareness and assist a person identify when to seek further support. Support provided under Component 1 should be available to all those who need it.
- Component 2 (selective or targeted): which makes provision for people to access more formal opportunities to reflect upon their grief, and may involve individual or group sessions, peer support, friendship groups, and/or specific groups relating to the type of bereavement, e.g. suicide.
- Component 3 (indicated): which encompasses specialist interventions that may involve mental health services, psychological support and specialist counselling.
This framework encompasses all of these components in the care required by bereaved people in Wales. It is important to note the inter-dependencies between each category and without adequate capacity being available in each component, subsequent components could become overwhelmed.
Other models or programmes of support
Similar programmes or models of support exist, particularly in relation to the needs of bereaved children, young people and their families/carers. A number of these evidenced based examples can be found in Annex 3.
9. Bereavement care to meet the needs of our population
While the informal care of friends, families and members of communities are invaluable, we recognise that there are those who live and are bereaved in situations where these supports are not available to them or are unable to meet their needs. One aspect of a public health approach to better supporting bereavement in Wales is provided by the encouragement of compassionate community values and principles.
The Welsh Government supports the work being undertaken by Compassionate Cymru, our NHS colleagues and many others across Wales to promote a wider conversation on caring for people at end of life, advance care planning, and 'what matters most' conversations, dying and bereavement. This framework is part of that overall activity.
The care received by those at the end of their lives and the people caring for them are key foci of Compassionate Cymru and supporting those who are bereaved is an important aspect of this work.
The Welsh Government’s Connected Communities – A strategy for tackling loneliness and social isolation and building stronger social connections (2020) further supports the Welsh Government’s ambition, working with statutory and third sector partners, to make Wales the world’s first compassionate country.
It recognises the need, as one of its 'Priorities for Action', to raise the profile of loneliness and social isolation as part of a £1.4 million Loneliness and Social Isolation Fund over the next three years. It also identifies how bereavement can be one of the life events which result in people feeling lonely or becoming socially isolated.
The Compassionate Cymru Steering Group, comprising a variety of statutory and third sector organisations is engaging with a range of key initiatives including Communities of Practice, social prescribers, community connectors and work by the Regional Partnership Boards, Public Service Boards, and other organisations to develop compassionate community models.
There are clear linkages between the establishment of Compassionate Cymru and the provision of community support to bereaved people in Wales. The role of the Social Value Forums, supported by the Regional Partnership Boards, will be key in working to identify, enhance and sustain the support communities are able to offer their residents during bereavement. The importance of supporting informal responses in this way is clear in the evidence already available around the ways in which well-being is enhanced by social connectedness. The benefits of this work will include the ability to target and make best use of the resources available from statutory and specialist services. Additionally encouraging events and resources which support and provide information around dying, death and bereavement can help build confidence in local community groups to support one another in bereavement and help to remove any stigma, which compromises people’s willingness to ask for and to offer help in bereavement. This is part of the role of Compassionate Cymru.
Person centred care should be holistic and include a spiritual, pastoral and religious dimension where this is required by the person (Health and Care Standards Wales 2015, p.8). Spiritual care addresses the dimension of illness, disability, suffering and importantly bereavement that go beyond the immediate and the physical. Chaplaincy provides specialist spiritual care (Standards for Spiritual Care Services in the NHS in Wales 2010) but importantly must link into or connect services between health care organisations and the multiple faith/pastoral communities within Wales.
10. Existing provision - scoping survey of bereavement services in Wales
In 2019, the Marie Curie Palliative Care Research Centre, Cardiff University, and the Wales Cancer Research Centre, funded by the End of Life Care Board in Wales, undertook a Bereavement Scoping Survey in Wales.
The survey identified that the amount of bereavement support available varied significantly across Wales. The findings identified gaps in the provision of adult and children and young people bereavement services, in particular following the loss of children, infants and in pregnancy, pregnancy loss and stillbirth. There are also gaps in provision of support in each of the NICE components above, including access to specialist support.
Its key considerations were as follows:
A National Framework: the development of a national framework for the delivery of bereavement care in Wales. This would in turn facilitate:
Prioritisation of Bereavement Care: the prioritisation of bereavement support at organisational and regional levels.
Equity and access to appropriate support: availability of appropriate types and levels of support which are responsive to local needs and comprise an effective balance of non-specialist community based provision and specialist professional intervention Referral and Risk Assessment: The establishment of clear referral pathways and approaches to risk/needs assessment. The development and maintenance of a directory of available bereavement provision could improve signposting, referrals and access to appropriate local support.
Training and Learning: Improved access to training for staff and volunteers and sharing of expertise and good practice between local service providers Evaluation and Assessment: Improvements in how services are evaluated and assessed, with implications identifiable for service improvement and investment. Appropriate sets of standards could be considered for use as audit and quality improvement tools, and suitable measures and methods identified for evaluating the impact of services on service users.
11. Learning from COVID-19
The impact of COVID-19, with shielding of 'at risk' groups which occurred during the first wave, the introduction of local lockdowns and necessary restrictions on meeting friends and family, has caused heightened levels of anxiety.
Additionally, changes to visiting policies across inpatient and care settings have limited contact with loved ones before and during death, complicating end of life care and contributing to the trauma of the bereaved. Restrictions have also affected how bereavement care is delivered, including across perinatal services.
The pandemic has highlighted the isolation felt by bereaved people, at a time when they needed support. It has also emphasised the need for bereaved families in a hospital setting to be allowed some dignity and to be able to spend some time with the deceased person, without feeling that the family were being rushed away.
Cardiff University are leading on a UK wide ‘Supporting People Bereaved during COVID-19 Study’, which is investigating bereavement experiences, support needs and support provision during the pandemic. Interim results have demonstrated the exceptionally difficult nature of pandemic bereavement and the unique sets of challenges experienced by people grieving at this time. Not being able to spend time with loved ones in their final illness, restrictions on numbers able to attend a funeral and the inability to console someone with a hug can be heart breaking for a bereaved person and their family. Grieving, already a lonely process is increasingly occurring in isolation without that contact from friends and family. For many communities, mutual social contact is an essential element of bereavement rituals, which allow for expression of grief and support of those bereaved. This has been especially difficult during the pandemic.
There is the sense from some bereaved people that their loved one’s death was avoidable. This coupled with a range of emotions including anger and frustration, with guilt in some cases that they themselves may have been complicit in transmitting the disease to their loved ones, is causing increasing distress.
All of these factors are having a lasting impact on people’s grief and there is a risk that this isolation, which many people are experiencing in the current environment, may lead to chronic loneliness. Just over half of participants in this study demonstrated 'severe' (28%), or 'high' (23%) levels of vulnerability in grief, as well as high/fairly high needs for support in 6 psycho-emotional domains. These included; dealing with feelings about being without loved ones (50%) and the way in which they died (60%); feelings of anxiety and depression (53%); expressing feelings and being understood by others (53%); feeling comforted and reassured (52%) and loneliness and social isolation (52%).
These phenomena have illuminated the need for bereavement support perhaps more than ever, however, we know that people were experiencing difficulties accessing support, for reasons such as long waiting lists, lack of appropriate support, and feeling uncomfortable asking for or not knowing how to access help pre pandemic. In seeking to improve bereavement care, we must learn from these experiences.
Many providers of bereavement support during the pandemic have moved to providing support by telephone or online rather than in person or in groups. This may not be the model preferred by bereaved people, but it is the prevailing model of support for the foreseeable future due to infection, prevention and control considerations for the bereaved person and the provider of support.
The National Bereavement Alliance Report, COVID-19: the response of voluntary sector bereavement services similarly highlights the impact of the pandemic on grief and bereavement. Key findings include the increased complexity of deaths, and subsequent increase in the levels of distress suffered by bereaved people, difficulties in accessing normal levels of support (e.g. family and friends) due to social distancing requirements resulting in increased isolation and loneliness, and lack of capacity in bereavement services.
We have learned during the pandemic that those with underlying conditions and those living in areas with high levels of social and economic deprivation have suffered disproportionately.
Learning from COVID-19 should provide foundations for the implementation of preventative initiatives that can make an impact on reducing all four harms. Bereavement support needs to be a core component in a national co-ordinated strategy on the response to a pandemic.
12. Black, Asian and Minority Ethnic communities
The report of the BAME COVID-19 Socioeconomic Subgroup chaired by Professor Emmanuel Ogbonna found that although the coronavirus pandemic has created widespread fears and risks to lives and livelihoods across communities in Wales and around the world, the impacts on Black, Asian and Minority Ethnic groups have been especially profound. Members from ethnic minority communities are disproportionately contracting and dying from the COVID-19 disease, with available statistics suggesting that British Black, Asian and Minority Ethnic groups are up to two times more likely to die from the disease than their white counterparts.
These losses have been exacerbated by the disruption caused by COVID-19 restrictions to the community resources, which would normally be available to them for informal support. Many families have not been able to visit dying loved ones, have had to grieve alone during lockdown and have experienced painful disruptions to funerals and traditional death rites.
The Cross Party Group on hospices and palliative care heard directly from bereavement service providers and leaders from Black, Asian and Minority Ethnic communities across Wales at their meeting on 20 January 2021.
The message from community leaders was clear: bereavement services are not always experienced as accessible to people from diverse communities, despite the efforts of bereavement services to ensure their services are open to all. Community leaders advised that tailored bereavement and mental health services are often needed to support people from ethnic minority communities and that people from ethnic minority communities should be involved in bereavement service design, taking a co-productive approach.
Similar views and experiences are described in a recent publication by BAMEStream, which reports results from a survey of Black, Asian and Minority Ethnic mental health services in the UK during the pandemic. The report identifies increased demand for bereavement support provided by Black, Asian and minority ethnic led organisations, as well as a need for mainstream Bereavement therapists and service providers to have quality assured cultural competency training. A need for research and good-practice sharing relating to ethnicity, bereavement and bereavement support provision is also identified.
The UK wide ‘Supporting People Bereaved during COVID-19 Study’ referenced in section 9 above aims to understand more about the bereavement experiences and support needs of people from minority ethnic backgrounds. Thirty-four participants from minority ethnic backgrounds took part in the survey, with follow up interviews planned to explore experiences in more depth. Research with voluntary sector bereavement services will also explore support provision relating to minority groups. A key goal of the study is to identify recommendations to ensure that equitable bereavement support is provided across the UK.
Providers and Commissioners of bereavement services need to engage with ethnic minority communities to address this inequity of care and to discuss what level of bereavement support is needed. Commissioners must ensure that this engagement and input to the bereavement support required, takes place. A bereavement standard has been introduced to monitor this.
13. Training, learning and supervision for individuals bereavement support
All formal volunteers and staff who come into contact with bereaved people should have the relevant training and experience for the level of support they offer (see Annex 1, section 1.2 for more detail on the types of support and the standards required). This will include initial training in listening skills, supporting the bereaved, identifying and providing the correct level of support at that time, identifying where further and more specialist support may be necessary, e.g. for more complex grief and other mental health conditions such as Post Traumatic Stress Disorder. Safeguarding training must be provided to all staff and volunteers.
There is a need to recognise that training in bereavement support (and other more specialist bereavement/end of life care support as required by their role), should also be made more widely available for those public facing non-clinical staff on the 'front line'.
Training needs should be established to ensure that staff and volunteers are equipped with the necessary skills and expertise, recognising that this may require training in other skills not just relating to counselling.
All providers should have mechanisms in place to review on a regular basis, the skills and competence of their staff and volunteers, and have a regular programme of continuing professional development to equip them with new skills, developments in the provision of bereavement support, and identifying where further training is required. The Bereavement Care Service Standards (statement 4) also highlight the need to provide access to support and supervision to ensure safe working practice and afford staff and volunteers the opportunity to recognise the impact of this work on them. Depending on the level of service provision, and the skill set of the provider, supervision should be undertaken in line with regulatory bodies, and in line with the Bereavement Care Service Standards.
As part of the implementation and ongoing support of the Bereavement Framework, a forum will be established to share experiences, ideas, best practice, and learnings.
14. Accessing bereavement support - the need for clear referral pathways
Bereaved people and their families looking for support at a time of distress need to be able to access up to date information concerning the range of support available, in a format that works for them. Bereaved people are often left 'floundering' with no indication of where to go for help, therefore timely and accurate information on how to access further support is of major importance.
Individual providers may be providing one or more levels of support but commissioners should ensure that all three levels are available and clearly signposted for professionals and the public.
On making contact with an organisation, the means of referral into the service needs to be clear with an understanding of the range of services available, including an estimate of the waiting time for that support, where a waiting list exists.
The provider needs to ensure that the process of assessment for referral into their service is clear and comprehensible, collecting only the information needed to ensure a full assessment of the needs of the bereaved person.
If after collecting this information and discussing the outcome of the assessment with the person, it becomes clear that their needs would be better served by another provider (in terms of complexity of need, specialism, type of service provision available, or more timely support), then onward referral to the alternative organisation should be offered to the bereaved person.
This onward referral could occur at the start of the bereavement support or during its initial stages, for example, after the bereaved person has been seen for the first time or first few sessions following a referral into the service.
Where, for example, a need for more specialist mental health provision has been identified then the referral into that service should be facilitated by primary care, although additional clinical information may be required including a mental health assessment by the Primary Mental Health team. (See Annex 1. Section 1.2 in relation to commissioners and providers’ responsibilities).
It will be important in any cases of onward referral for both organisations (both referring and receiving) to ensure that the process is properly managed, that the bereaved person does not feel “forgotten”, and that they are still able to access support in the intervening period.
There will also be times (such as throughout the pandemic or following mass bereavement) when services should proactively reach out to communities to offer bereavement care and support. This is particularly important for those communities who may find it difficult to access support, see Section 10.
15. Self-management/care
Health, social care, third sector partners and service users are central to the planning, design and delivery of bereavement services.
Approaches, which empower people to manage their own bereavement such as self-help guides, can be highly effective. Health and care staff will need to adopt these approaches to increase quality of outcomes and experience for individuals and to maximise access to resources and reduce variation across services. Services will need to assess and plan to prioritise those in most urgent need and to consider meeting potential increased demand.
Ensuring that bereavement is 'everyone’s business' will support the use of self-management and wider community resources to increase general health and well-being. Signposting to sources of support should be part of all bereavement after care, and professionals should be aware of the range of online and other services and the various community groups that can offer support.
Professionals suggesting self-management will need to ensure that there has been appropriate assessment of the risk and that clinical intervention is not required.
16. Securing outcomes
Although grief can be complex whatever the last stage of the person’s life has been like, we know that experiences and perceptions of poor communication, of poor care, or of uncontrolled distress can make bereavement much harder. Mitigating the distress of the bereaved is only one reason to provide good end of life care, most of which is beyond the scope of this framework, but the approach to bereavement has to be matched by attention to the care of those with chronic and progressive life shortening illnesses and the care of the dying. Family involvement and memory making during all parts of the care pathway, as well as during end-of-life care, is particularly important alongside good care of the person nearing the end of life.
To optimise bereavement outcomes will require good bereavement care throughout the system, grounded in supportive communities, to complement this good clinical care. Strong interdisciplinary and partnership working throughout health, social care, third and independent sectors will make best use of the resource available.
The implementation of this framework will entail adoption of evidence-based person reported outcome measures and other measures of services. These will help to identify gaps and inequities and will support development and delivery of services that are equitable and responsive to people’s needs.
17. Links to other work/programmes
18. Role of the National Bereavement Steering Group
In order for Wales to meet the bereavement needs of the population, action is needed at national, regional and local level.
The End of Life Care Board has overall responsibility for bereavement care and support in Wales and through the National Bereavement Steering Group will provide the ongoing leadership and oversight that is needed to implement this framework and to support regional and local planning. This will include:
- Monitoring implementation of the bereavement standards (Annex 1) and advising the Welsh Government on further action/resources needed
- Working with health boards, local authorities, regional partnership boards and other public bodies to improve bereavement care and support
- Considering the specific bereavement needs of Black, Asian and Minority Ethnic communities and other communities who are more likely to be affected by the impacts of health inequalities
- Supporting the development and/or implementation of clear referral pathways for specific client groups
- Supporting bereavement providers to deliver identified national bereavement outcome measures for adults and children/young people
- Developing quality standards for the design and delivery of national training, education and information programmes to ensure bereavement is 'everyone’s business', promoting an empowering, person-centred approach that is adopted by all
- Embedding advances in technology and smarter ways of working to support the increased demand for bereavement support and improve access, outcomes and experience
- Training and up-skilling the wider multidisciplinary and multiagency teams, promoting self-management and the co-production of care alongside access to a range of specialist bereavement provision.
Promoting and encouraging recognition of the importance of community based approaches to offering support and information as the first resource available to all.
Annex 1 – Bereavement standards
The need for bereavement support (including anticipatory grief/pre-bereavement) has already been identified. It is important for those commissioning bereavement services, those providing the service, and for bereaved people who will ultimately receive that service to have confidence that there are measures in place to ensure that (a) support is available to them and (b) that it meets the required standard. The National Bereavement Alliance, in its document A Guide to Commissioning Bereavement Services in England gives a description of what good local provision for bereaved children and their parents and carers looks like (shown here to illustrate models of delivery).
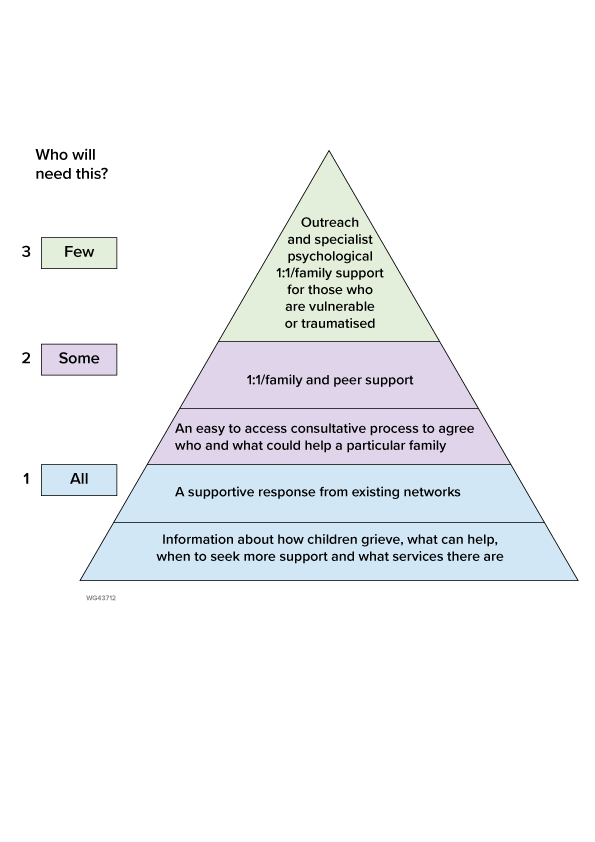
1.1 Government
Welsh Government will be responsible for monitoring implementation of the bereavement standards listed at 1.2.
1.2 Commissioners
(a) Commissioners should ensure that the appropriate standard of care and support can be provided to children, young people and adults, so that their bereavement needs can be met taking into account their faith, culture, gender, economic status, and their location within Wales. This includes supporting bereaved people to understand how children grieve.
(b) Commissioners should ensure that anyone experiencing a bereavement is provided with up to date, timely and relevant information on the support available to them. This includes ensuring that bereaved people are able to access up to date information concerning the support available to them in Welsh.
(c) Commissioners should ensure that bereavement support is available to those people who may find it difficult to access bereavement support (e.g. because of disability including people who are sight-impaired and/or hearing impaired) or who are in groups who have historically been under represented (e.g. LGBTQ+), members of Black, Asian, and Minority Ethnic Communities. Commissioners will be responsible for engaging with these communities and groups to ensure that the bereavement support available meets their requirements.
(d) Commissioners should ensure that people’s risk of adverse bereavement outcomes is assessed at the initial point of assessment in a service.
(e) Commissioners should ensure that bereavement services, which may already exist within their individual Health Board Directorates, are properly co-ordinated to provide a consistent level of service to bereaved people.
(f) Commissioners should ensure that all bereavement support, including all information at first point of contact, any referral conversations and information collected, assessments, which may be carried out, leaflets, materials and support sessions whether, provided face to face or virtually, should always be available in Welsh.
(g) Commissioners should ensure that support is provided in other languages, including British Sign Language, where required. This includes commissioning access to interpretation and translation services to ensure that the support can be provided.
(h) Commissioners should demonstrate that adequate support is available under each of the following categories:
| Category | Type of support | Standard required |
|---|---|---|
|
Available to all bereaved people (NICE component 1 Universal) |
Commissioners’ responsibilities: To ensure that sufficient informal care, support networks and information services are available, and that the information provided is always up to date, and in a range of formats and languages. Providers’ responsibilities: Information about bereavement and support available, outlined as part of a conversation with the bereaved person or a family member. Material provided via leaflets or details of on-line resources given. Ascertain what support can be provided through informal social networks. Some providers may also directly enable social/peer support by hosting social activities or groups. |
Accurate and timely Information on how to deal with practical matters. Information on grief and coping with bereavement to be made available Sign-posting on how to access other types of support to be understood. |
|
Available to some bereaved people (NICE component 2 Selective/Targeted) |
Commissioners’ responsibilities: To ensure that capacity exists to support bereaved people who request it, especially for those people who may be at risk of developing more complex needs. Providers’ responsibilities: People supported to reflect upon their/their children’s grief, individually or within a group environment. Support via befriending/faith/other community groups, as appropriate to the individual circumstances; trained bereavement support workers. |
See core standards, s1.3 below and s1.4 detailed measures |
|
Available to a small number of bereaved people (NICE component 3 Indicated) |
Commissioners’ responsibilities: To ensure that specialist support is available, and accessible. To identify those people who may be at risk because of complex needs or from the effects of long term or complicated grief. This would include the effect of grief on a child/young person’s emotional neuro psychological development). Providers’ responsibilities: To ensure that the appropriate level of expertise is in place to meet this high level of need, where specialist interventions are required. |
See core standards, s1.3 below and s1.4 detailed measures |
1.2.1 Identification of baseline standards
Commissioners will be asked for their initial views on their plans to monitor the bereavement standards once the framework is published. They will also be requested to indicate their current level of compliance against the standards using the following measures on an annual basis:
(a) standard not in place
(b) standard already in place
(c) standard in progress
Where a standard is already in place, Commissioners will be asked for the existing measurements in place, which they use to demonstrate compliance, including both quantitative and qualitative feedback from users.
1.2.2 Monitoring of standards
Welsh Government will use the existing performance management structures that are in place to monitor Commissioner’s compliance with these standards. This will be undertaken through the NHS Delivery framework, the future National Outcome Framework for Health and Social Care, and require NHS organisations to self-assess and culminate in reports being produced for the NHS Chief Executives.
1.3 Core standards for providers of bereavement services
(a) The following are core standards which providers of bereavement support are expected to follow, and be able to demonstrate as part of a regular review of services. They are designed to be clear, concise and comprehensive and should be used for planning, provision and quality review of all bereavement care.
They are taken from the Bereavement Care Service Standards, 2014 produced by the Bereavement Services Association and Cruse Bereavement Care, and endorsed by the National Bereavement Alliance, following funding from the Department of Health. They are the fundamental principles for the provision of bereavement care services:
Confidentiality: services should respect the confidentiality and privacy of each bereaved person and any information shared by them, with due regard to safeguarding, consent and data protection.
Respect: services should respect the individuality of each bereaved person’s grief and needs, with each person treated with compassion and sensitivity.
Equality and Diversity: services should be non-discriminatory and delivered without prejudice, recognising and responding to personal beliefs and individual situations including (but not exclusive to) age, culture, disability, gender, sexuality, race, religion and spirituality (Equality Act 2010).
Quality: services should ensure that all those delivering support to bereaved people, whether in a paid or voluntary capacity, have the skills, knowledge, training, supervision and support relevant to their role, and that services work to improve what they offer.
Safety: services should have robust processes for recruitment, including appropriate levels of clearance with the Disclosure and Barring Service and ongoing staff/volunteer development. There needs to be due regard to safe and ethical practice in order to protect bereaved people and those who work with them. The necessary processes for safeguarding must be in place and accountability evidenced through an audit trail.
Bereavement support is underpinned by a variety of standards, including professional standards set by their own organisation, or professional body. In addition, there may be other standards and outcomes measurements to meet local requirements, or as required by funders or as part of service level agreements or other commissioning documents.
1.4 Detailed measures for bereavement support providers
Providers of bereavement support should consider adopting some or all of the following measures, or such other measures as agreed with their funders.
1.4.1 Access to the service
(a) Registration/Referral: Following an enquiry from a bereaved person, initial contact should be made within five working days.
(b) Risk Assessment: A comprehensive assessment of the needs of the bereaved person and a risk assessment must be undertaken by a trained individual with the required skills. This may include arranging higher priority support for those people deemed to be at the highest risk, or referring the client for more specialist support elsewhere.
(c) Waiting times for support: an estimate of the approximate waiting time should be provided on initial registration with the service. This is intended to give a general guideline only on the time it may take for support to be provided.
(d) Keeping in touch: where bereaved people are on a waiting list for support, regular contact should be maintained to provide re-assurance and check that their situation has not changed. This should occur at a minimum of four weekly intervals and if it is identified that more timely support could be provided by an alternative provider, then this should be discussed and an onward referral to the alternative service offered.
(e) Review: If after a period of twelve weeks support is still awaited, a discussion with the bereaved person should take place to discuss their current situation, their needs after three months and whether support can be provided from an alternative source.
1.4.2 Monitoring of the service provision
(a) Supervision and monitoring: all services provided must be monitored to ensure the safety of the client and the provider of that support, and that they are operating ethically.
(b) End of support evaluation: a process must be in place to monitor the quality of the service provided with both quantitative (e.g. using recognised evaluation tools such as the Clinical Outcomes in Routine Evaluation CORE-10) and qualitative (e.g. questionnaires for completion at the final session of support) measures. There are other tools which may be used as required (CORE 10 is not appropriate for young children therefore other evaluation tools must be used).
(c) Evaluation measures: These should include client perception of waiting times, ease of initial contact and or subsequent referral, understanding of client needs and level of empathy shown, adequacy of support given, understanding of next steps and/or referral to other support where appropriate.
1.4.3 Review
The needs of bereaved people, articulated by colleagues in Welsh Government’s Patient Experience team, together with research from palliative and bereavement care will be included in the review and updating of these measures.
1.5 Using the bereavement standards
Commissioners will be responsible for implementing these standards at regional and/or local level. Providers of bereavement care will be responsible for implementing these standards at the organisational level.
Annex 2 – Membership of the National Bereavement Steering Group
| Member | Title | Organisation |
|---|---|---|
|
Dr Idris Baker (Chair) |
National Clinical Lead Palliative/End of Life Care |
End of Life Care Board |
|
Gareth Hewitt |
Head of Older People’s Health |
Welsh Government |
|
Alison Lott |
Senior Manager, Older People’s Health |
Welsh Government |
|
John Moss |
National Bereavement Lead |
Welsh Government |
|
Vivienne Collins |
Policy Manager, Older People’s Health |
Welsh Government |
|
Gareth Howells |
Nursing Officer |
Welsh Government |
|
Professor Lesley Bethell |
Chair |
Compassionate Cymru Steering Group |
|
Daisy Shale |
Medical Examiner Officer Lead |
Medical Examiners Service, Wales |
|
Janette Bourne |
Director |
Cruse Bereavement Care Cymru |
|
Anita Hicks |
Clinical Lead |
Sandy Bear’s Children’s Bereavement Charity |
|
Helen French |
Hospices Representative |
City Hospice |
|
Claire Cotter |
National Co-ordinator for Suicide and Self-harm Prevention |
NHS Wales collaborative |
|
Jessica Reeves |
Public Affairs and Campaigns Manager |
SANDS (Still Birth and Neonatal Death Society) |
|
Jessica Evans |
Patient experience representative |
Fair Treatment for the Women in Wales |
|
Sue Phelps |
Director |
Alzheimer’s Society |
|
Ian Stevenson |
Chair and Senior Nurse |
All Wales Spiritual Health and Well-being Group |
|
Dr Emily Harrop |
Research Associate. Marie Curie Palliative Care Research Centre. |
Cardiff University |
|
Dr Anthony Byrne |
Clinical Director of the Marie Curie Palliative Care Research Centre. |
Cardiff University |
|
Josie Anderson |
Campaigns and Policy Manager |
Bliss |
|
Alex Walsby |
Senior Nurse Bereavement |
Hywel Dda University Health Board |
|
Rocio Cifuentes |
Chief Executive Officer |
Ethnic Minorities and Youth Support team Wales |
|
Melanie Lewis |
End of Life Care Co-ordinator |
NHS Wales Collaborative |
|
Charity Garnett |
Palliative Care Nurse for North Powys and Bereavement Project Co-ordinator |
Powys Teaching Health Board |
|
Jane Brewin |
Chief Executive Officer |
Tommy’s |
|
Rhian Mannings, MBE |
Founder and Chief Executive Officer |
2 Wish Upon a Star |
|
Dr Anne Johnson |
Consultant Clinical Psychologist General Paediatrics |
Aneurin Bevan University Health Board |
|
Dr Liz Gregory |
Consultant Clinical Psychologist |
Aneurin Bevan University Health Board |
|
Sally Rees |
National third Sector Health and Social Care Facilitator |
WCVA |
|
Marika Hills |
Strategic Partnership Manager, Wales |
Macmillan Cancer Support |
|
Professor Stuart Todd |
Life Science and Education Department |
University of South Wales |
|
Dr Karen Pardy |
General Practitioner |
Cardiff South West Cluster |
|
Dr Rachel Lee |
General Practitioner |
Cardiff South West Cluster |
Annex 3 – Bereavement models
This annex provides examples of both bereavement models and frameworks currently operating within the UK.
3.1 Children’s bereavement
The following models outline the differing needs of 'most' 'some' and 'few' children, and how these needs can best be met, and by whom.
The Childhood Bereavement Network, in conjunction with the National Children’s Bureau, has published guidelines on what good provision looks like, as well as what constitutes high quality support.
The Irish Childhood Bereavement Framework: encourages adults who care for bereaved children to understand that, in most situations, children can be supported by providing accurate information and emotional support through their family and community: Standards for supporting bereaved children and young people
3.2 Pregnancy and baby loss bereavement
The National Bereavement Care Pathway (NBCP) for pregnancy and baby loss is a pathway to improve the bereavement care parents in England receive after pregnancy or baby loss. The nine NBCP bereavement care standards were launched during Baby Loss Awareness Week 2018. They form the basis on which the roll out programme in England is established.
National bereavement care pathway
National bereavement care pathway - standards
3.3 Bereavement by suicide
Developing and delivering local bereavement support services is a toolkit produced by the National Suicide Prevention Alliance and the Support after Suicide Partnership, supported by Public Health England. The documents provide guidance for developing and delivering local bereavement support services, and guidance on evaluating local bereavement services. A common resource used across the UK to support people bereaved by suicide is ‘Help is at Hand’, which is available in English and Welsh on the Dewis Cymru website.
National suicide prevention alliance
NICE guidance specific to bereavement by suicide
Resources for traumatically bereaved children (UK Trauma Council)
Annex 4 - Links to other guidance/frameworks/supporting documents
Audiology framework 2017 to 2020
Guidance on funerals: COVID-19
Maternity services strategy (2019 to 2024)
Suicide and self harm prevention strategy 2015 to 2022
Quality statement 5: Supporting people bereaved or affected by a suspected suicide
Mental health delivery plan 2019 to 2022
Loneliness and social isolation (connected communities)
Substance misuse delivery plan: 2019 to 2022
Statutory guidance to Welsh local authorities on the provision of independent counselling services
Sensory loss communication needs: data standards (WHC/2018/030)
Annex 5 - Glossary of terms
| Term | Description |
|---|---|
|
Anticipatory grief |
Where a person can experience grief before a death, perhaps at the point of a diagnosis being received. |
|
Bereavement |
Experienced in relation to the death of a person wherever and whenever it happens. |
|
Blue light workers |
Emergency services such as the police, fire and ambulance staff who use blue flashing lights to either respond to an emergency call out or take someone to a hospital. |
|
BSL |
British Sign Language (Sign Language) is a visual means of communicating using gestures, facial expression, and body language. It is used mainly by people who are deaf or have hearing impairments. |
|
CORE |
The Clinical Outcomes in Routine Evaluation (CORE) system comprises tools and thinking to support monitoring of change and outcomes in routine practice in psychotherapy, counselling and any other work attempting to promote psychological recovery, health and wellbeing. |
|
Disenfranchised Grief |
Where a person’s grief may remain hidden because they feel it is not accepted or acknowledged by others. |
|
LGBTQ+ |
Lesbian, gay, bisexual, transgender, queer (or sometimes questioning), and others. The 'plus' represents other sexual identities including pansexual and Two-Spirit. |
|
Medical Examiners |
Medical examiners are senior medical doctors who undertake medical examiner duties, outside of their usual clinical duties. They are trained in the legal and clinical elements of death certification processes. |
|
NBCP |
The National Bereavement Care Pathway (NBCP) seeks to increase the quality of, and reduce the inequity in, the bereavement care provided to parents in England by healthcare professionals. |
|
NHS |
The National Health Service (NHS) is the umbrella term for the publicly funded healthcare systems of the United Kingdom. |
|
NICE |
National Institute for Health and Clinical Excellence (NICE) is an organisation that seeks to improve outcomes for people using the NHS and other public health and social care services through the production of evidence-based guidance and quality standards and performance metrics. |
|
Post Traumatic Stress Disorder |
Post Traumatic Stress Disorder (PTSD) is a mental health condition that develops following a traumatic event characterised by intrusive thoughts about the incident, recurrent distress/anxiety, flashback and avoidance of similar situations. |
|
Public Service Boards |
Public Services Boards (PSBs) improve joint working across all public services in each local authority area in Wales. Each board must carry out a wellbeing assessment and publish an annual local wellbeing plan. The plan sets out how they will meet their responsibilities under the Well-being of Future Generations (Wales) Act. |
|
RPBs |
Regional Partnership Boards (RPBs) bring together health boards, local authorities and the third sector to meet the care and support needs of people in their area. |
